Medical term:
Lupus
lupus
[loo´pus]It was once thought that this was a fairly rare disease, but improved immunologic testing procedures have shown that it is not. It is primarily a disease of women, occurring five to ten times more often in females than in males. Although the peak incidence is between 30 and 40 years of age, the condition has also been diagnosed in the very young and the very old.
SLE is the classic prototype of autoimmune disease of connective tissue. Its etiology is unknown, but the high level of autoantibodies in persons with the condition indicates a defect in the regulatory mechanisms that sustain self-tolerance and prevent the body from attacking its own cells, cell constituents, and proteins. Patients with SLE can have a wide variety of autoantibodies against nuclear and cytoplasmic cellular components. The presence of high levels of antinuclear antibody (ANA) in SLE patients with glomerulonephritis indicates a pathogenic role for that antibody. The antibodies are directed against deoxyribonucleoprotein, DNA, histone, and a soluble non–nucleic acid molecule called Sm antigen.
Factors that appear to contribute to the development of SLE include exposure to sunlight or ultraviolet radiation from sunlamps, a genetic predisposition to the disease, certain drugs, viral infections, and hormonal influences.
Clinical manifestations of SLE are confusingly diverse owing to the involvement of connective tissue throughout the body. Typically, the patient seeks medical help for relief of fever, weight loss, joint pain, the characteristic butterfly rash, pleural effusion and pleuritic pain, and nephritis. The detection of ANA by microscopic immunofluorescence is supportive evidence for the presence of SLE.
Either glomerulonephritis, which is usually mild, or cardiovascular manifestations such as myocarditis, endocarditis, or pericarditis, are found in about half the patients with SLE. Pulmonary disease, especially pleurisy, is also relatively common, as are gastrointestinal disturbances and lymph node involvement. Organic neurologic disturbances produce behavioral aberrations and frank psychosis in some patients; in a few others, there are peripheral neuropathies, motor weakness, and diplopia.
Supportive measures are used to prevent or minimize acute relapses and exacerbations of symptoms. The patient is instructed to avoid exposure to sunlight and ultraviolet radiation from other sources, blood transfusions, penicillin, and the sulfonamides. Active disease is treated with topical steroids, nonsteroidal antiinflammatory drugs for fever and joint pain, corticosteroids, and immunosuppressants. The goal of drug therapy is suppression of the immune system. Treatment of specific manifestations of SLE is aimed at prevention of complications. Physical therapy may be required to alleviate muscle weakness and prevent orthopedic deformities.
lu·pus
(lū'pŭs),lupus
(lo͞o′pəs)lupus
(1) Lupus erythematosus:• Discoid lupus erythematosus;
• Systemic lupus erythematosus, see there.
(2) Cutaneous tuberculosis (lupus vulgaris).
lu·pus
(lū'pŭs)lupus
(loo'pus) [L. lupus, wolf]discoid lupus erythematosus
Abbreviation: DLETreatment
The patient should avoid exposure to the sun. Skin lesions should be treated with topical corticosteroids, but overuse of these preparations should be avoided.
drug-induced systemic lupus erythematosus
lupus erythematosus
neonatal lupus
lupus panniculitis
Lupus profundus.lupus pernio
lupus profundus
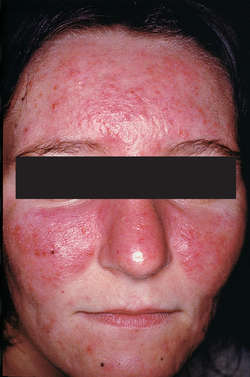
systemic lupus erythematosus
Abbreviation: SLEEtiology and Pathology
SLE is classified as an autoimmune disease in which the body seems to be unable to maintain normal mechanisms of tolerance to autoantigens. Activation of T helper cells and B cells results in the production of autoantibodies that attack antigens in the cytoplasm and nucleus of cells and on the surface of blood cells. The exact cause of SLE is unknown: genetic defects, hormonal changes, infection, physical or mental stress, some drugs, immunizations, and environmental triggers (sunlight, UV light exposure) are possible predisposing factors. See: autoimmune disease; glomerulonephritis
Autoantibodies can react with autoantigens to form immune complexes in such large numbers that they cannot be completely excreted; the immune complexes may precipitate within blood vessels, producing inflammation at the site and disrupting the flow of blood and oxygen to tissues. These deposits are particularly damaging in the glomeruli. Autoantibodies also promote the destruction of cells by stimulating neutrophil and macrophage phagocytic activity, which increases cell destruction from trauma, infection, or drugs.
Diagnosis
In 1997, revised criteria for diagnosis of SLE were established. The diagnosis can be made if four or more of the following criteria are present, either at one time or sequentially: (1) butterfly rash; (2) raised, scaly discoid skin lesions; (3) abnormal titer of antinuclear antibodies seen by immunofluorescence; (4) other autoantibodies (anti-Sm; serological tests for syphilis); (5) pleuritis or pericarditis (together referred to as “serositis”); (6) hemolytic anemia, leukopenia (white blood cell count less than 4,000 mm3), lymphopenia (lymphocyte count less than 1,500/mm3), or thrombocytopenia of less than 100,000/mm3; (7) oral or nasopharyngeal ulcers; (8) nonerosive arthritis; (9) psychosis or seizures without other clear cause; (10) photosensitivity skin rash; and (11) proteinuria greater than 0.5 g/day or cellular casts in the urine.
Some drugs can cause a lupus-like syndrome; the most common of these are procainamide, isoniazid, and hydralazine. See: drug-induced systemic lupus erythematosus
Symptoms
The onset of the disease may be acute or insidious. Patients have a wide variety of clinical symptoms, signs, and laboratory findings, but anemia, thrombocytopenia, polyarthritis, (polyarthralgia) skin rashes, glomerulonephritis, fever, malaise, weight loss, fatigue, and low blood levels of complement are the most common. Other signs include pleuritis, pericarditis, myocarditis, neurological changes including behavioral changes and seizure activity (neural lupus), gastrointestinal ulcerations, Raynaud's phenomenon (present in about 20% of patients), and other problems caused by inflammatory changes of the blood vessels or connective tissue. Most patients are prone to infection.
Treatment
No cure for SLE exists, and complete remission is rare. About 25% of patients have mild disease, demonstrating only minor skin and hematological signs, and can be treated with nonsteroidal anti-inflammatory drugs for their arthritis symptoms and topical treatment (sometimes with corticosteroid creams) for skin lesions. Rashes may respond to antimalarials, e.g., hydroxychloroquine, but patients must be observed closely for the possibility of drug-induced retinal damage. Other treatments for skin rash include quinacrine, retinoids, and dapsone. Life-threatening and severely disabling conditions should be treated with high doses of corticosteroids and supplemental calcium to minimize osteoporosis, which may be an undesired side effect of long-term glucocorticoid use. Immunosuppressive drugs are used for severe exacerbations and to reduce steroid dosage.
Prognosis
The prognosis depends on which organ systems are involved, how severely they are damaged, and how rapidly the disease progresses. Ten-year survival rates are high (80%). Renal failure and infections are the most common causes of death.
Patient care
Patient education related to the disease, diagnostic procedures, and treatment is essential in lupus, as in any chronic disease. Ongoing assessment is carried out to assess flares of the illness. The purpose, proper dosage, use, and side effects of drugs is taught. Patients need emotional support to help cope with changes in appearance. Patients should be taught to wear clothing and hats that block direct sunlight, use a sunscreen with a 15 or higher protection factor, and to maintain a diet appropriate for their renal functional status. The health care professional should help establish a regimen for adequate relief of both the musculoskeletal pain and chronic fatigue experienced by most patients, encouraging adequate rest. Heat packs relieve joint stiffness and pain, and regular gentle exercise helps to maintain full range of motion. Physical and occupational therapy consultations are provided as appropriate. Additional support and teaching depend on the organ system most affected by the disease. If the female patient of childbearing age has no renal or neurologic impairment, she can have a safe, successful pregnancy if desired. Over time, patients with severe progressive disease need assistance in coping with chronic illness and the possibility of mortality. Referrals to the Lupus Foundation of America (202-349-1155; www.lupus.org) and the Arthritis Foundation (800-283-7800; www.arthritis.org) are helpful.
lupus vulgaris
lupus
A general and imprecise term referring to one of a variety of severe skin disorders, especially LUPUS VULGARIS.Lupus (systemic lupus erythematosus or SLE)
lu·pus
(lū'pŭs)Patient discussion about lupus
Q. What is Lupus? My best friend has been diagnosed with Lupus. What is it? Is it contagious?
Q. how long do u live with lupus? why do we get lupus? why was i hit with it along with all my other medical problems? i dont understand why..
Q. Is a rash a symptom of lupus? My Sister has lupus for several years now. I recently developed a rash on my face. Is this a symptom of lupus? Could I have also been infected with this disease?
Latest Searches:
zincoid - zinciferous - zincalism - Zinaxin - Zinacef - Zimulti - Zimmerlin - Zimmermann - zimelidine - Zimany - Zilver - zileuton - zilantel - Zila - Zika - zigzagplasty - Zieve - Ziemssen - Zielke - Ziehl -
- Service manuals - MBI Corp